
Anaphylaxis Response Simulator
⚠️ The Five-Minute Rule Calculator
Calculate how quickly risk increases based on delayed administration.
Risk Increase: 0%
Risk jumps by 44% for every minute beyond the initial window.
💉 Administration Technique Practice
Protocol Complete
You have practiced the standard administration sequence. Remember: Outer thigh, bare skin, hold tight.
Every second counts when a child goes into anaphylactic shock. In those critical first five minutes, the difference between life and death often comes down to one decision: do you give epinephrine, or do you wait? Too many people hesitate. They worry about looking foolish if it’s just a mild allergy. They fear legal trouble. Or worse, they simply don’t know how to use the device properly. This hesitation isn’t just scary-it’s deadly. Studies show that for every minute epinephrine is delayed beyond the initial five-minute window, the risk of severe outcomes jumps by 44%. That’s not a statistic; that’s a preventable tragedy.
We need to talk about Epinephrine Auto-Injector Training is a standardized educational protocol designed to equip caregivers, school staff, and emergency responders with the skills to recognize anaphylaxis and administer life-saving medication correctly and quickly. It’s not just about watching a video once a year. It’s about building muscle memory so that when panic sets in, your hands know what to do without thinking. With nearly 1 in 13 children having food allergies, this skill is no longer optional-it’s a public health necessity.
The Five-Minute Rule: Why Timing Is Everything
Anaphylaxis is a rapid, full-body allergic reaction that can close your airways and drop your blood pressure dangerously low. The body doesn’t send a warning shot before it shuts down. According to data from the Journal of Allergy and Clinical Immunology, 95% of deaths from anaphylaxis occur within 48 hours, but the most critical period is the first few minutes after symptoms start. Epinephrine works by constricting blood vessels and relaxing muscles in the lungs, effectively reversing the shock state. But it only works if it gets into the bloodstream fast enough.
The American Academy of Allergy, Asthma & Immunology emphasizes that administration should happen ideally within five minutes of symptom onset. Why five minutes? Because that’s the window where the drug can stop the cascade of histamine release before organ damage begins. Waiting to see if antihistamines like Benadryl work is a dangerous mistake. Antihistamines are too slow and don’t treat the life-threatening aspects of anaphylaxis, such as throat swelling or hypotension. Your job isn’t to diagnose the severity perfectly; your job is to act on the presence of multiple symptoms-hives plus vomiting, or difficulty breathing plus dizziness-and inject immediately.
Mastering the Device: Technique Matters More Than You Think
You might think giving an injection is simple: stick it in and press. But AUVI-Q is an epinephrine auto-injector brand that requires specific handling steps, including removing caps in a precise order and holding the device against the thigh for ten seconds devices, and others like EpiPen, have distinct mechanisms. Using them incorrectly means the dose never enters the muscle, rendering the entire effort useless. A common error seen in drills is injecting through clothing. Fabric can block the needle or absorb the medication. The injection site must be bare skin.
Here is the correct technique for most adult and older child doses (66+ pounds):
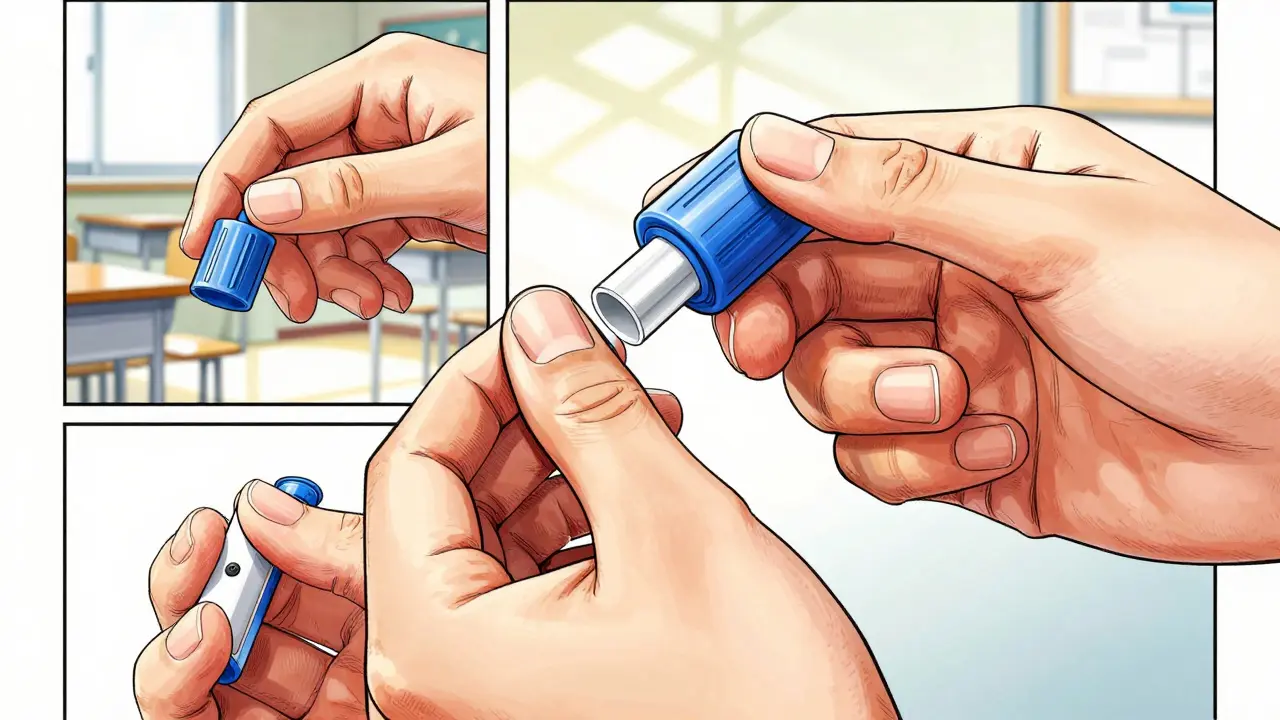
- Identify the end: Hold the injector with the blue cap (or safety cap) pointing up and the needle end pointing down. Do not confuse these ends.
- Remove the right cap: Pull off the blue safety cap first. Never pull the needle-end protector until you are ready to inject.
- Select the site: Aim for the outer mid-thigh. The lateral thigh has large muscle groups that absorb the medication quickly. Avoid the front of the thigh or areas near bone.
- Inject firmly: Swing the device and jab it hard into the outer thigh at a 90-degree angle. Push until you hear a click.
- Hold tight: Keep the device pressed against the thigh for the required time. For AUVI-Q, hold for 10 seconds. For EpiPen, hold for 3 seconds. Count it out loud if you’re nervous.
- Massage: After removing the device, massage the area for 10 seconds to help absorption.
Notice the emphasis on "outer thigh." Injecting into the inner thigh or buttocks can lead to slower absorption or accidental injection into a blood vessel, which increases the risk of side effects without improving efficacy. Also, remember that pediatric devices exist for smaller children. Always check the weight limit on the package. If you’re unsure, err on the side of caution and call emergency services while preparing the appropriate device.
Training Gaps: Why Knowledge Alone Isn’t Enough
Reading a pamphlet does not make you competent. Research from the Food Allergy Research & Education organization shows that programs incorporating hands-on practice with trainer devices reduce administration errors by 78% compared to lecture-only formats. Yet, many schools and workplaces still rely on passive learning. The problem is psychomotor skill decay. Without physical repetition, the fine motor skills needed to remove caps and aim correctly fade rapidly. One study found that untrained individuals took an average of 2 minutes and 17 seconds to administer epinephrine correctly during their first drill. After three practice sessions, that time dropped to 48 seconds. That’s a massive difference in a life-or-death scenario.
Another major gap is symptom recognition. Up to 83% of fatal anaphylaxis cases involve a failure to administer epinephrine because bystanders misidentified symptoms as mild. A child scratching their nose isn’t necessarily having a severe reaction, but a child who scratches their nose, then starts coughing, then vomits, is likely escalating toward anaphylaxis. Training must explicitly teach the difference between mild localized reactions and systemic ones. Mild reactions might include hives on one arm. Severe reactions involve two or more body systems: skin (hives), respiratory (wheezing), gastrointestinal (vomiting), or cardiovascular (dizziness/palpitations). If two systems are involved, inject immediately.
Legal Protections and Overcoming Fear
Fear is a real barrier. Many staff members hesitate because they worry about being sued if they accidentally injure someone or if it turns out to be a false alarm. This fear is understandable but misplaced. All 50 states in the US have Good Samaritan laws that protect individuals who act in good faith during emergencies. Furthermore, specific legislation like California Education Code Section 49414 and Illinois Public Act 099-0711 explicitly protects school personnel who administer epinephrine according to protocol. You cannot be held liable for administering epinephrine in good faith during an apparent medical emergency. The liability for *not* acting when action was required is far greater.
Employers and schools also benefit from clear protocols. Having a written safety plan reduces ambiguity. When everyone knows their role-who calls 911, who retrieves the injector, who stays with the patient-the response becomes smoother and faster. Documentation is key. Keep records of training completion and ensure that stock epinephrine is checked regularly for expiration dates. Expired epinephrine loses potency over time, though it may retain some activity for months past its date. Still, always prioritize fresh medication.
| Brand | Dosage | Hold Time | Key Feature |
|---|---|---|---|
| EpiPen | 0.3 mg / 0.15 mg | 3 seconds | Most widely recognized brand |
| AUVI-Q | 0.3 mg / 0.15 mg | 10 seconds | Audio instructions guide user |
| Veyo | 0.3 mg / 0.15 mg | 3 seconds | Slender design, easy grip |

Post-Injection Care: The Job Isn’t Done Yet
Once the epinephrine is delivered, the crisis isn’t over. Adrenaline wears off in 10 to 20 minutes. This is why biphasic reactions occur-where symptoms return after the initial improvement. Monitoring is crucial. Lay the person flat with their legs elevated unless they are having trouble breathing, in which case let them sit up. Cover them with a blanket to maintain body temperature and prevent shock. Check their airway, breathing, and heart rate every five minutes.
If symptoms persist or worsen after five minutes, and paramedics haven’t arrived, administer a second dose using a different auto-injector. About 16-35% of anaphylaxis cases require a second dose. Never reuse a single device. Even if it feels empty, there might be residual medication, but it won’t be a full therapeutic dose. Always have two injectors available for any high-risk individual. Call emergency services immediately after the first injection. Epinephrine is a bridge to professional care, not a cure-all.
Building a Culture of Preparedness
Preventing errors starts long before an emergency occurs. Schools and organizations should implement quarterly refreshers. Skill retention drops to 47% after six months without practice. Use expired devices for drills-they look and feel identical to new ones but are safe to handle. Encourage open discussions about fears and uncertainties. When staff members feel supported, they act faster. Designate multiple trained personnel per campus. Don’t rely on just one nurse or teacher. Spread the responsibility so that coverage is constant.
Finally, advocate for better training standards. Push for hands-on components in all certification programs. Demand that your workplace provides realistic trainer devices. Ask questions during training sessions. Understanding the "why" behind each step makes the "how" stick. Remember, you are the first line of defense. Your confidence saves lives.
How long does epinephrine last in the body?
Epinephrine typically lasts for 10 to 20 minutes. This short duration is why monitoring is essential and why a second dose may be necessary if symptoms return or fail to improve. Always seek immediate medical attention even if the person seems better.
Can I inject epinephrine through clothing?
No, you should not inject through clothing. Fabric can interfere with the needle penetration or absorb the medication, leading to ineffective dosing. Always expose the outer mid-thigh skin before administration.
What if I’m afraid of making a mistake?
It is better to act than to hesitate. Good Samaritan laws protect those who act in good faith during emergencies. The risk of anaphylaxis progressing to cardiac arrest far outweighs the risks of incorrect administration. Practice with trainer devices to build confidence.
Do I need to massage the injection site?
Yes, massaging the site for 10 seconds after injection helps distribute the medication in the muscle tissue, potentially speeding up absorption. However, do not massage if the needle is still embedded; remove the device first.
When should I give a second dose?
Administer a second dose if symptoms persist or worsen after five minutes and emergency medical services have not yet arrived. Use a separate auto-injector for the second dose.

Justina Ingram
May 17, 2026 AT 06:59omg this is so scary 😱 i mean like really terrifying tbh. my cousin almost died last year because her teacher was too scared to use the epi pen lol. she just sat there watching him sweat instead of acting and it took forever for anyone to step up. people need to stop being such wimps about liability or whatever excuse they come up with. its better to inject someone by accident than let them choke on their own throat while you debate the legal ramifications ugh. seriously yall get trained already its not that hard 🙄