Imagine waking up with skin that feels like it's on fire, only to find that a simple change in the weather or a new brand of soap has triggered a massive breakout. For millions of people, this isn't a rare occurrence-it's the daily reality of Atopic Dermatitis is a chronic inflammatory skin condition characterized by dry, itchy, and inflamed skin resulting from a compromised skin barrier function and immune dysregulation. Also known as eczema, it affects up to 30% of children and 10% of adults globally. The goal isn't just to stop the itching once it starts, but to fundamentally change how you protect your skin to prevent the next flare from happening.
Why Your Skin Reacts: The Science of the Barrier
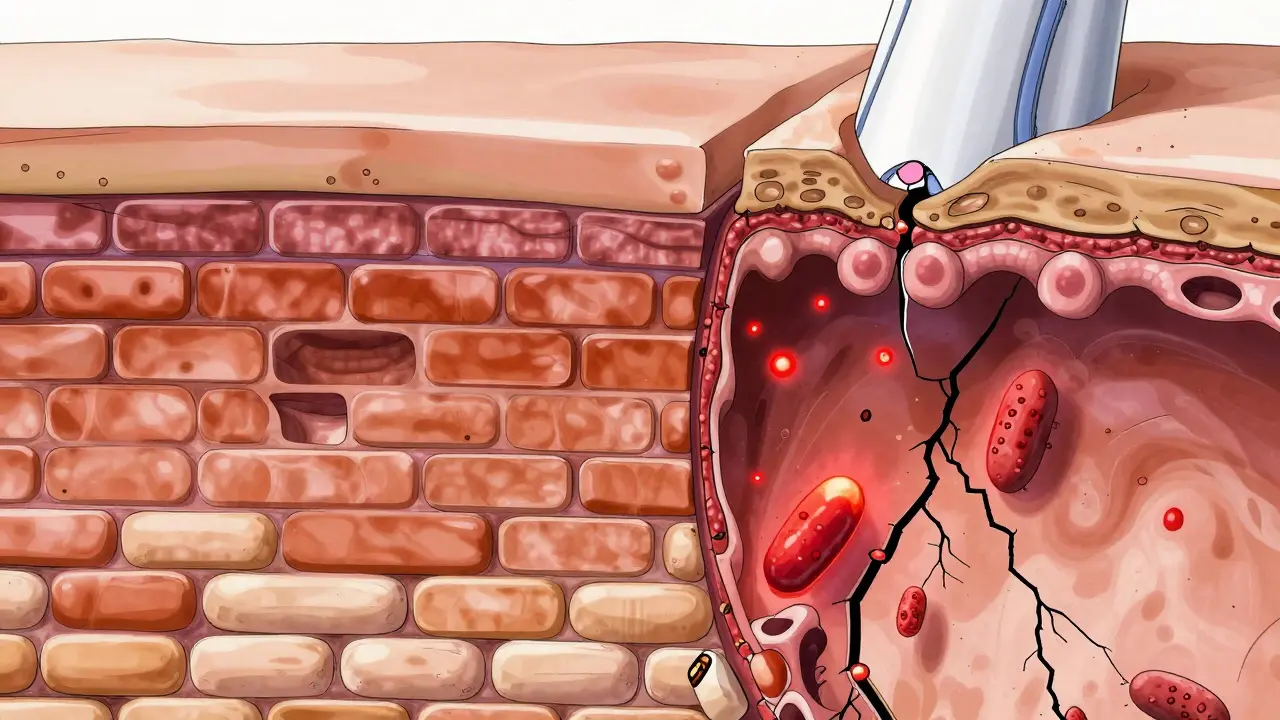
To understand why triggers cause flares, we have to look at the skin's "brick and mortar" system. In healthy skin, the bricks are skin cells and the mortar is a mix of lipids. For many with AD, there's a genetic glitch involving the Filaggrin gene. This protein is crucial for creating a natural moisturizing factor. When it's missing or mutated-which happens in up to 50% of severe cases-the skin can't hold onto water.
This leads to a spike in transepidermal water loss (TEWL). While healthy skin loses a small amount of moisture, AD skin can lose up to three times as much. This creates microscopic cracks in the skin, leaving the door wide open for irritants, allergens, and bacteria like Staphylococcus aureus to seep in, triggering the immune system and causing that familiar, intense itch.
Common Flare Triggers You Need to Track
Not every trigger is the same for everyone, but most fall into a few predictable categories. If you aren't tracking your flares, you're guessing at your treatment. Here are the most common culprits:
- Climate and Humidity: Cold, dry air is a major enemy. When humidity drops below 40%, the risk of a flare jumps by about 37%. Conversely, heat above 80°F (27°C) can cause sweat-induced irritation for nearly 70% of patients.
- Chemical Irritants: Be wary of Sodium Lauryl Sulfate (SLS). Even at low concentrations of 0.5%, this common foaming agent in soaps can strip your barrier and cause immediate inflammation.
- Fragrances and Preservatives: Around 15% of people with eczema react poorly to artificial scents. Additionally, preservatives like methylisothiazolinone can cause contact dermatitis in a small but significant percentage of users.
- The Itch-Scratch Cycle: This is a physical trigger. Scratching releases more inflammatory chemicals, which makes you itch more, which leads to more scratching. Breaking this loop is the primary goal of therapy.

The Essentials of Emollient Therapy
If steroids treat the fire, Emollient Therapy is the fireproofing. Emollients are lipid-based moisturizers designed to seal the skin barrier, reduce water loss, and soothe inflammation. They aren't just "lotions"; they are medical tools that fall into three main categories:
| Type | Key Ingredients | Main Benefit | Best For... |
|---|---|---|---|
| Occlusives | Petrolatum (Vaseline), Lanolin | Forms a physical seal to stop water loss | Severe dry patches, nighttime use |
| Humectants | Glycerin, Hyaluronic Acid | Pulls water from deeper layers to the surface | Hydrating the skin throughout the day |
| Barrier Repair | Ceramides, Fatty Acids | Replenishes missing lipids in the skin | Long-term maintenance and prevention |
For the best results, a combination approach is usually best. Using a humectant to add moisture and then "locking it in" with an occlusive like petrolatum-which has a 98% efficacy rate in reducing water loss-is the gold standard for severe flares.
How to Apply: The "Soak and Seal" Method
Applying cream haphazardly isn't enough. Timing and technique are everything. Dr. Amy Paller emphasizes that the 3-minute window after bathing is critical; applying moisturizer within this timeframe can lock in 50% more moisture than waiting until the skin is dry.
- The Bath: Take a lukewarm bath or shower for 15-20 minutes. Avoid hot water, which strips natural oils.
- The Pat-Down: Gently pat your skin with a towel. Leave the skin slightly damp.
- The Seal: Apply your emollient immediately. Use downward strokes-following the direction of hair growth-to avoid irritating follicles.
- The Dosage: Don't be stingy. Research shows that adults using over 100g of emollient weekly have 43% fewer flares than those using less. For most adults, 250-500g per week is the recommended target.

Managing the Burden: When Emollients Aren't Enough
Despite the benefits, many people struggle with the "greasiness" of these products, leading about 30% of patients to stop using them within six months. If you hate the feel of heavy creams, try applying them right before bed or using a ceramide-based cream during the day, which often absorbs faster than pure petroleum jelly.
It is also important to recognize when emollients need backup. While they are great for maintenance, they usually only clear 30-40% of mild cases on their own. For moderate-to-severe flares, you'll likely need Topical Corticosteroids or calcineurin inhibitors like tacrolimus for sensitive areas. In extreme cases, systemic treatments like Dupilumab are used to target the immune response directly.
Pro Tips for Long-Term Control
Consistency is the hardest part of AD management. To make it easier, keep a "moisture station" in your bathroom and bedroom so the product is always within reach. If you're on a budget, remember that simple petrolatum is often more effective and significantly cheaper than expensive, fragranced boutique creams.
Keep an eye out for new developments. Sustained-release ceramides are now entering the market, offering longer-lasting hydration that can reduce the number of times you need to reapply during a busy workday.
Can I use any moisturizer from the drugstore?
Not necessarily. Many drugstore moisturizers contain fragrances or alcohols that can trigger a flare. Look for products labeled "fragrance-free" and "hypoallergenic." Brands like CeraVe, Eucerin, and Cetaphil are often recommended because they include ceramides and avoid common irritants.
Why does my skin still itch even after applying cream?
If you're in the middle of a flare, emollients might not be enough to stop the itch because they treat the barrier, not the active inflammation. You may need a topical steroid or an anti-inflammatory medication to calm the immune response before the moisturizer can effectively maintain the skin.
Is it safe to use petrolatum every day?
Yes, petrolatum is one of the safest and most effective occlusives available. It has a very low risk of causing allergic reactions compared to complex creams with multiple preservatives.
How often should I be moisturizing?
Twice-daily application is the clinical recommendation. Consistent use can reduce the frequency of flares by up to 36% over six months.
Does diet affect eczema flares?
While environmental triggers like weather and soap are more direct, some people find certain foods trigger inflammation. However, focusing on skin barrier repair through emollients is generally the most effective first-line strategy regardless of diet.

Carol Yang
April 25, 2026 AT 20:19The soak and seal thing is a total game changer once you actually stick to it!
Edwin Perez
April 27, 2026 AT 16:19Sure, follow the 'science' of big pharma creams. They just want you addicted to the grease so you don't notice the chemicals they're pumping into the water supply to trigger these flares in the first place. It's all a cycle to sell more tubes of petrolatum.
Michael Chukwuma
April 28, 2026 AT 23:36I really appreciate the breakdown of the different types of emollients. It's kind of overwhelming when you're staring at a shelf of twenty different creams and don't know if you need a humectant or a barrier repair one. This makes it way easier to manage.
Hayley Redemption
April 30, 2026 AT 04:52Imagine thinking a generic drugstore brand is a 'medical tool'. The reduction in TEWL is basic dermatology, but suggesting that 500g of grease a week is a sustainable lifestyle for a functioning adult is laughable at best and insulting at worst. Some of us actually have to wear clothes that aren't made of absorbent cotton.
Eric Mwiti
April 30, 2026 AT 07:50Right, because applying a pound of Vaseline to my body every week is exactly how I wanted to spend my adulthood. Truly a glamorous existence.
Ben Jima
May 2, 2026 AT 00:14While the greasiness is a challenge, focusing on the 3-minute window after a shower is the most effective way to see results quickly. If you're struggling with the residue, try applying the occlusives only at night and sticking to the ceramide-based creams during the day. It keeps the skin protected without ruining your wardrobe!
Nila Sawyer
May 3, 2026 AT 02:20Oh my goodness, this is such a wonderful and detailed guide for everyone struggling with their skin! 🌟 I've always felt so lost when looking at ingredients but seeing the distinction between humectants and occlusives really opens my eyes to how I can better care for my family and friends who are suffering too! It's just so inspiring to see the science explained in a way that feels accessible and encouraging for all of us, and I honestly believe that with a little bit of consistency and a lot of love for our skin, we can all get through these flare-ups together! Keep shining and keep sharing this amazing knowledge! ✨💖🌸
William Zhigaylo
May 3, 2026 AT 16:01The lack of emphasis on the psychological toll of chronic itching is a glaring omission here. It is an absolute nightmare to deal with the sleep deprivation caused by the itch-scratch cycle, and simply applying a 'medical tool' does nothing to address the systemic failure of the healthcare system to provide immediate relief for severe cases. This guide treats a debilitating condition as if it were a mere inconvenience of dry skin, which is utterly unacceptable and reductive.
Brittney Prince
May 5, 2026 AT 03:46Typical. They tell you to buy more creams while they ignore the fact that these 'fragrance-free' brands still use preservatives that mess with your hormones. It's all a scam anyway.
Vijay AGarwal
May 6, 2026 AT 22:22STOP EVERYTHING! 🛑 You absolutely MUST try the soak and seal method immediately if you haven't already! I have seen people go from complete misery to total skin salvation just by changing the timing of their moisturizer! It is an absolute revolution in skincare! The difference between applying on dry skin versus damp skin is like night and day-it's literally the secret weapon we've all been missing!
Elle Torres Sanz
May 8, 2026 AT 11:55It's great to see different options listed here because everyone's skin is so unique. Some people might find the heavy occlusives too much, but for others, they are a lifesaver. We should all just support each other in finding what works for our own bodies without judgment.
Beena Garud
May 9, 2026 AT 09:27One must contemplate the duality of the skin as both a shield and a gateway. The fragility of the Filaggrin protein serves as a poignant reminder of the intricate and often precarious balance of our biological existence. It is truly humbling to realize how a single molecular deviation can lead to such profound physical distress.
sachin singh
May 10, 2026 AT 19:57The mention of sustained-release ceramides is quite intriguing. I believe this technology could significantly improve the quality of life for those who find frequent reapplication burdensome throughout the day.
Karyn Tindall
May 11, 2026 AT 00:24I literally cannot handle the feeling of petroleum jelly on my arms during the summer! It's a total nightmare! I feel like I'm melting into a giant slip-and-slide and I just can't deal with it!